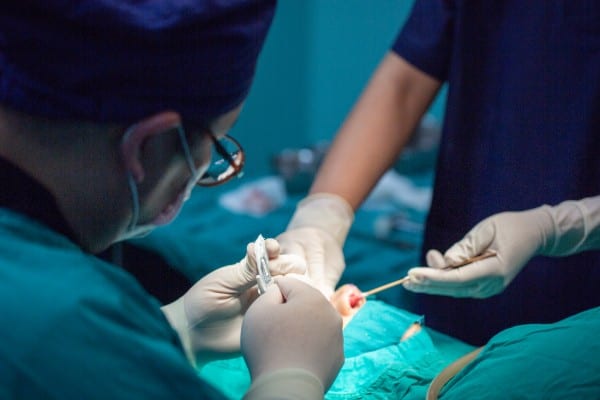
In the last few days, Dr. Yumiko Kadota’s story of the brutal hours and dehumanising conditions she experienced as a Plastic and Reconstructive Surgery registrar at Bankstown Hospital in Sydney hit headlines.
This aspiring surgeon has exposed the appalling conditions and untenable hours she worked as an unaccredited registrar at Bankstown Hospital. https://t.co/qvSkBpnRFM via @smh
— Kate Aubusson (@Kaubo) February 5, 2019
Doctors, politicians and the general public are now grappling with the notion that medicine, a purportedly caring profession, can mistreat each other badly.
It is of particular surprise to those who come from outside medicine, who care not just about the capable doctor at the heart of this story, but also their own health. Will their doctor be safe to care for them?
Overwork is common to many industries. The 2016 census showed that Australians were continuing to work longer and longer hours, with half of all workers putting in around 50 hours a week. Overwork is endemic in business and in trade. In medicine it can be particularly severe.
My take on #Miko'story:
What are the 3 main causes of #burnout?
1. Work overload
– Case load
– Work hours/schedule2. Under staffing
3. Feeling underappreciated
Who controls the above 3?
INSTITUTIONAL LEADERSHIPSelfcare is not the answer. https://t.co/ODZ0ho0YxG
— #JennyFromTheBlock (@jennybencardino) February 5, 2019
It is 2010 and I am a surgical registrar.
“Did you hear that the registrar at x hospital crashed his car driving home last night?” a surgeon asks me. I express concern for my colleague, thinking about how I barely manage to keep my eyes open driving home most days. “They need to adjust better, otherwise they aren’t really cut out for a surgical career,” the surgeon concludes, as if fatigue has a muscle which can be worked out and built up.
In medicine, we talk about hours a fortnight, because our rosters and timesheets are done fortnightly. As an intern, I learned that it is considered acceptable to work eighty hours in a week if you have the following week off, and not be paid overtime for the week worked because the average across the fortnight is only forty.
A frank and frightening view of medical training at its darkest; the exploitation of the unaccredited registrar – the worst bit? She isn’t alone. She’s just speaking up. #ditlyf #mh4docs @RACSurgeons https://t.co/DBG5LcggEq
— Tessa Kennedy (@drtessak) February 3, 2019
Kadota was working 140-160 hours a fortnight, with many consecutive days on call. The latter involves receiving phone calls throughout the night, but this is not ‘work’ and does not count towards ‘hours worked’.
This has shocked doctors and health ministers alike. And yet, many doctors can point to our ‘biggest fortnight’. For me, it was 204 hours in twelve consecutive days, with the majority of it on call, in the midst of a job where the average was 180 hours a fortnight. I was in my third trimester of pregnancy.
Why do these hours exist, and why has it been so resistant to change? At the heart of the problem is a health system which has too many patients to treat for the resources that are put into it.
Elective surgery waiting lists across the country are enormous, and emergency cases need to be fit in around them. Cancel elective cases to do an emergency and old Mrs. Smith, who has already waited five months to have her skin cancer treated, waits another six weeks. All the while it is growing.
Hospitals are financially penalised for not meeting elective surgery targets, and so emergency cases must be done after hours, when staffing is markedly reduced. While patients wait, surgical registrars argue with each other over whose patient deserves care first, because there is only one operating theatre to do it in.
In a specialty like plastic surgery, patients can often be discharged immediately after they have had their surgery. There is increased pressure on registrars to stay late and get cases done. The same pressures apply to non-surgeons to admit, treat and discharge patients, regardless of the hour. The hospital needs the bed for someone else, otherwise it will be penalised for exceeding waiting times in the Emergency Department. The consequence is overtime, especially for the junior doctors at the coalface of this system.
In the midst of this genuine health care need is the pyramid scheme that our health system runs on, a large base of doctors aspiring to certain specialties, and a limited number of positions, often employed as locums or on short term contracts.
With the carrot of hope and the promise of future employment, hospitals can take the best of our junior doctors’ labour, because training programs ask them to compete with each other in an ongoing battle royale for a coveted training position. Governments underfund hospitals, administrators underfund units, heads of unit ask the impossible of their juniors, whether they want to or not.
Whose fault is this? No-ones. Everyones.
It is 2015 and I have completed my training, determined to make life better for those coming behind. One of my registrars approaches me with a simple problem. The hospital does not provide parking. She is nervous walking many blocks to her car at 2 am. I can fix this!
I escalate the issue, but there is no parking available, and administration is not concerned. “She can ask security to escort her,” they say, except she has to wait an hour for a security escort because they are busy too, and at 2 am she just wants some sleep.
She is not on a training program, so I cannot appeal to the Royal Australasian College of Surgeons or a training board, who might take interest in her welfare. She is a member of the Australian Medical Association but she does not want to call them because she fears their intervention will eliminate her chances of success in the battle royale, and she does not have a job for next year yet. She does not want to become ‘tainted’. She decides that in balance she will accept the risk.
I realised then why even the kindest surgeons I had worked with as a trainee had not seemed to help. Even senior surgeons are powerless in the face of administrative hierarchy and jurisdictional confusion to solve simple problems.
I cannot get her a car park; the idea that I can stop her from needing to be there in the middle of the night is laughable.
Sydney hospital faces trainee ban over junior doctor scandal https://t.co/UGfZut9jyS via @smh thanks to @jilltomlinson and @drtessak for strong comments. AMA is lucky to have you both.
— Fiona Davies (@FionaDavies8) February 5, 2019
The only weapon we have is to shut down the service until the situation is rectified – but we are doctors first, and denying care to patients seems far more reprehensible than denying care to ourselves. Even our junior doctors would not ask for that.
It is 2018 and I am speaking to an administrator in a private hospital. They ask me what I think of operating late into the night like some of my colleagues, and I tell them that I have no interest in doing so.
They pause and ask me if I think it is safe that some colleagues are there until 2 am. I ask them to look up data on safety and fatigue. The effects of fatigue on performance and safety are explicitly clear, and yet, as a profession, we think that we have somehow cheated that.
Some doctors work too hard years after they have to. No-one stops them. Private and public hospitals benefit from it.
There are stories of the doctor who sleeps in their car; the doctor who never says ‘no’; the doctor who has not had a weekend off in several years. These are told as stories of strength and valour, not as stories of a broken system. We have adjusted to a new normal where the lens of fatigue limits our ability to see that this is dangerous and wrong. I see now how my lecturer in 1998 could say that working forty hours a week was part-time without a hint of irony.
Kadota’s story has jolted us awake, momentarily. We see in this moment that those hours are not just numbers on a time sheet, but have unacceptable consequences on individuals. Just as we have wrung our hands and discussed many times before.
And while it is reassuring that presidents of medical Colleges, our peak advocacy groups and a Health Minister have expressed their shock and outrage, and I am proud that they have genuinely sought to change conditions at this institution and make reparations to this individual, this moment is only one of many and is nothing new.
We carry a suicide rate double that of the general population, and we have this conversation every time we lose another colleague forever. This is the first week of the new medical training year, and thousands of unnamed doctors have signed up to rosters just like hers, in a system that devalues and dehumanises them.
I don’t know if this will be the moment that all stakeholders will come together to finally fix this broken system so that it is not dependent on individual good will. But what I do know is that each and every one of us can ask each other today – regardless of hierarchy, and without judgment or consequence – whether we are ok, whether we are safe, and whether we are #RestedDocs.